Macular Degeneration Symptoms, Detection & Latest Treatments
Executive Summary: Early detection of macular degeneration can preserve vision for decades. With breakthrough 2025 treatments, including gene therapy and stem cell research, plus proven preventive strategies, maintaining central vision is more achievable than ever.
Approximately 19.8 million Americans aged 40 and older live with some form of age-related macular degeneration (AMD), with 1.49 million having the vision-threatening late-stage form, making it the leading cause of vision loss among older adults. While this statistic appears concerning, recent advances in macular degeneration early detection methods and revolutionary AMD treatment options emerging in 2025 have significantly improved the outlook for preserving central vision.
Understanding macular degeneration symptoms and recognizing early warning signs represents a critical factor in maintaining vision quality over time. Whether individuals are experiencing subtle visual changes or seeking proactive eye health protection, this comprehensive analysis examines current knowledge regarding macular degeneration early detection, established AMD treatment options, and emerging therapeutic developments.
What is Macular Degeneration? Understanding the Basics
Macular degeneration affects the macula, a specialized retinal region measuring approximately 5.5 millimeters in diameter, responsible for central visual acuity and fine detail perception. This anatomical structure functions as the eye’s primary high-resolution imaging center, enabling activities requiring visual precision, including reading, facial recognition, driving, and detailed manual tasks.
When AMD develops, progressive deterioration of central vision occurs while peripheral vision typically remains preserved. This pattern of vision loss, while not resulting in complete blindness, significantly impacts activities of daily living that require fine visual discrimination.
Dry vs Wet Macular Degeneration: Key Differences
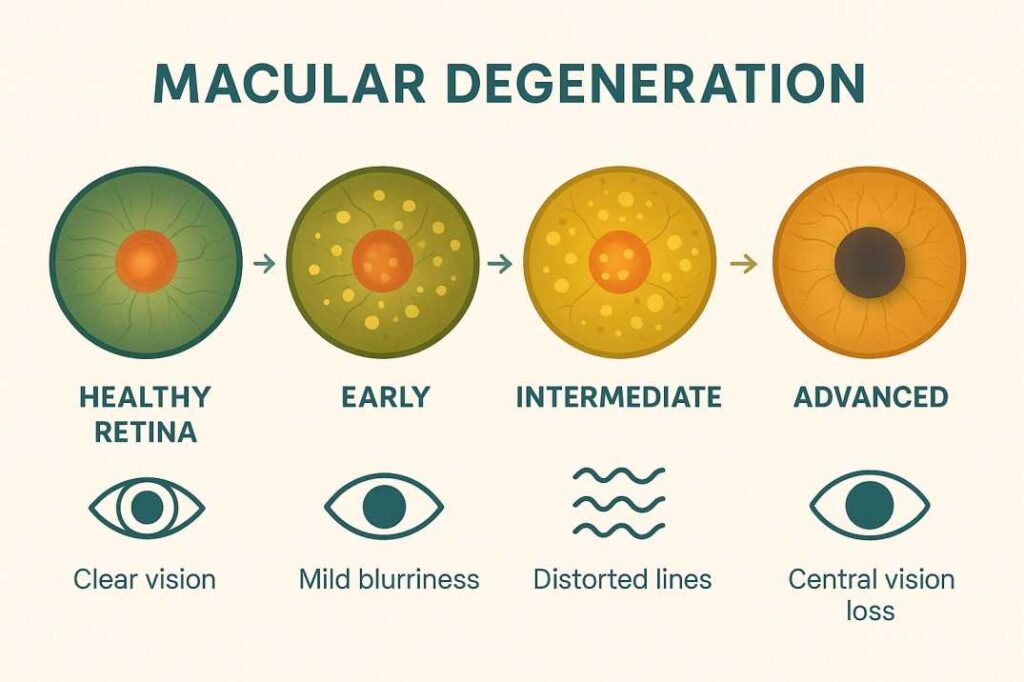
Dry Macular Degeneration (Atrophic AMD) Dry AMD represents approximately 85-90% of all macular degeneration cases, characterized by a gradual progression over multiple years. The pathophysiology involves the accumulation of extracellular deposits called drusen beneath the retinal pigment epithelium, subsequently leading to macular atrophy. The condition progresses through three distinct phases:
- Early Stage: Small drusen (≤63 micrometers) with minimal visual impact
- Intermediate Stage: Medium to large drusen (≥125 micrometers) with possible mild visual symptoms
- Advanced Stage (Geographic Atrophy): Significant retinal pigment epithelium and photoreceptor loss resulting in central scotoma formation
Wet Macular Degeneration (Neovascular AMD) Although representing only 10-15% of AMD cases, wet AMD accounts for approximately 90% of severe vision loss from the condition. This form develops when pathological choroidal neovascularization occurs, with abnormal blood vessels penetrating through Bruch’s membrane and proliferating beneath the neurosensory retina. These vessels demonstrate increased permeability, leading to hemorrhage, exudation, and rapid central vision deterioration.
Macular Degeneration Early Detection: Your First Line of Defense
The most significant factor in preserving your vision is catching macular degeneration in its earliest stages. Since early AMD symptoms often produce no noticeable changes, regular comprehensive eye examinations are essential, especially if you’re over 50 or have AMD risk factors for the disease.
Evidence-Based Risk Factor Assessment
Contemporary research identifies multiple modifiable and non-modifiable risk factors that influence AMD development and progression.
Modifiable Risk Factors:
- Tobacco use: Confers a 2-3 fold increased risk through oxidative stress and vascular compromise
- Dietary factors: High saturated fat intake and low antioxidant consumption correlate with increased AMD prevalence
- Obesity: Particularly abdominal adiposity, associated with inflammatory cascade activation
- Cardiovascular disease: Hypertension and atherosclerosis compromise choroidal perfusion
- Ultraviolet light exposure: Cumulative lifetime exposure contributes to retinal oxidative damage
- Physical inactivity: Sedentary lifestyle correlates with increased AMD risk
Non-Modifiable Risk Factors:
- Age: Risk increases exponentially after age 55, with prevalence exceeding 30% by age 75
- Genetic predisposition: Family history confers a 3-6 fold increased risk
- Gender: Female individuals demonstrate higher AMD prevalence, particularly post-menopause
- Ethnicity: Caucasian populations show the highest susceptibility compared to other ethnic groups
Contemporary Diagnostic Methodologies for Early AMD Detection
Advanced retinal imaging technologies have transformed early macular degeneration detection capabilities, enabling identification of pathological changes years before symptomatic manifestation:
Optical Coherence Tomography (OCT) High-resolution, non-invasive cross-sectional retinal imaging providing quantitative assessment of retinal layer thickness, drusen characteristics, and geographic atrophy progression. Current spectral-domain and swept-source OCT systems achieve axial resolutions of 3-7 micrometers, facilitating detection of subtle macular architectural changes.
Fundus Autofluorescence (FAF) Specialized imaging technique utilizing lipofuscin fluorescence properties to visualize retinal pigment epithelium metabolic activity. Abnormal autofluorescence patterns often precede structural changes visible on conventional fundoscopy, providing early biomarkers for AMD progression.
Adaptive Optics Scanning Laser Ophthalmoscopy Emerging technology enabling cellular-level retinal visualization, allowing direct assessment of photoreceptor integrity and retinal pigment epithelium morphology in vivo.
Multimodal Imaging Integration. Contemporary diagnostic protocols combine multiple imaging modalities to provide comprehensive macular assessment, improving sensitivity and specificity for early AMD detection.
Clinical Presentation and Symptom Recognition
While early AMD frequently remains asymptomatic, progressive disease manifestation includes specific visual disturbances that warrant immediate ophthalmological evaluation:
Early-Stage Symptoms:
- Reduced scotopic visual function (difficulty with low-light conditions)
- Subtle metamorphopsia (mild visual distortion)
- Decreased contrast sensitivity
- Impaired color discrimination
Intermediate to Advanced-Stage Symptoms:
- Central scotoma development (blind spots in the central visual field)
- Significant metamorphopsia with straight line distortion
- Reduced visual acuity affecting reading and detailed tasks
- Compromised facial recognition capability
Clinical Emergency Indicators: Acute onset of the following symptoms necessitates urgent retinal specialist consultation within 24-48 hours:
- Sudden metamorphopsia development
- Rapid central vision deterioration
- New central scotoma formation
- Acute color perception changes
Research demonstrates that wet AMD patients receiving anti-VEGF therapy within 48 hours of symptom onset achieve significantly superior visual outcomes compared to delayed treatment initiation.
Current AMD Treatment Options: Evidence-Based Approaches
Treatment strategies vary significantly between dry and wet macular degeneration, with wet AMD having more established therapeutic interventions.
Evidence-Based Treatment Protocols for AMD Management
Contemporary treatment approaches vary significantly between AMD subtypes, with wet macular degeneration having established therapeutic interventions, while dry AMD management has recently expanded with FDA-approved options.
Therapeutic Interventions for Dry Macular Degeneration
Nutritional Pharmacotherapy The Age-Related Eye Disease Studies (AREDS and AREDS2) represent landmark clinical trials demonstrating significant therapeutic benefit from targeted nutritional supplementation. The evidence-based AREDS2 formulation includes:
- Ascorbic acid (Vitamin C): 500mg
- α-tocopherol (Vitamin E): 400 IU
- Lutein: 10mg
- Zeaxanthin: 2mg
- Zinc oxide: 80mg
- Cupric oxide: 2mg
Clinical outcomes demonstrate approximatelya 25% reduction in progression to advanced AMD among intermediate-stage patients over 5-year follow-up periods.
FDA-Approved Complement Inhibitors for Geographic Atrophy. Recent therapeutic advances have introduced complement cascade inhibition for advanced dry AMD treatment:
- Pegcetacoplan (SYFOVRE): C3 complement inhibitor demonstrating 20% reduction in geographic atrophy growth rate
- Avacincaptad pegol (Izervay): C5 complement inhibitor with a similar efficacy profile
Both medications require intravitreal administration at 4-6 week intervals and carry specific risk-benefit considerations requiring specialist evaluation.
Wet Macular Degeneration: Anti-VEGF Therapeutic Protocols
Intravitreal Anti-VEGF Therapy Anti-VEGF medications represent the current standard of care for neovascular AMD, demonstrating superior efficacy compared to previous therapeutic modalities. These pharmacological agents inhibit vascular endothelial growth factor, thereby reducing pathological angiogenesis and vascular permeability:
First-Generation Agents:
- Bevacizumab (Avastin): Humanized monoclonal antibody, molecular weight 149 kDa, off-label use
- Ranibizumab (Lucentis): Antibody fragment, molecular weight 48 kDa, FDA-approved 2006
Second-Generation Agents:
- Aflibercept (Eylea): VEGF-trap recombinant fusion protein, molecular weight 115 kDa
- Brolucizumab (Beovu): Single-chain antibody fragment, molecular weight 26 kDa
- Faricimab (Vabysmo): Bispecific antibody targeting VEGF-A and angiopoietin-2
Clinical Efficacy and Outcomes: Randomized controlled trials demonstrate maintenance or improvement of visual acuity in >90% of patients receiving regular anti-VEGF therapy. Real-world effectiveness studies indicate approximately 50% visual stability due to suboptimal treatment adherence and injection frequency variations.
Photodynamic Therapy (PDT) Less commonly used today, PDT combines a light-activated drug with laser treatment for specific types of wet AMD lesions.
Laser Surgery: Traditional laser photocoagulation is now rarely used due to the superior outcomes with anti-VEGF therapy.
Emerging Therapeutic Modalities and Research Developments (2025)
Contemporary macular degeneration research encompasses multiple innovative approaches, from genetic interventions to regenerative medicine, representing potential paradigm shifts in AMD management.
Gene Therapy for Neovascular AMD
Vector-Mediated Anti-VEGF Production Gene therapy approaches aim to establish sustained intraocular anti-VEGF production, potentially eliminating the need for repeated intravitreal injections. Current investigational protocols include:
RGX-314 (REGENXBIO): Adeno-associated virus vector delivering anti-VEGF transgene via subretinal or suprachoroidal injection. Phase III clinical trials (ATMOSPHERE and ALTITUDE studies) are evaluating long-term safety and efficacy compared to standard anti-VEGF therapy.
ADVM-022 (Adverum Biotechnologies): Intravitreal AAV-mediated gene therapy demonstrating sustained anti-VEGF expression in Phase II trials, though development has been suspended pending safety evaluation.
Stem Cell-Based Regenerative Therapies
Retinal Pigment Epithelium Replacement. Multiple research groups are investigating stem cell-derived RPE transplantation for geographic atrophy treatment:
iPSC-Derived RPE (National Eye Institute): Autologous induced pluripotent stem cell-derived retinal pigment epithelium patches are being evaluated in Phase I/IIa trials for geographic atrophy treatment.
RPESC-RPE-4W (Luxa Biotechnology): Proprietary retinal pigment epithelial stem cell therapy demonstrated mean visual acuity improvement of 21.67 letters at 12-month follow-up in Phase I/IIa trials.
Extended-Duration Treatments
Port Delivery System (Susvimo) Genentech’s rice-grain-sized implant continuously delivers anti-VEGF medication for up to six months, dramatically reducing injection frequency.
High-Dose Formulations Eylea HD provides four times the standard dose at approximately $2,600 per injection, potentially extending treatment intervals to 3-4 months for many patients.
Combination Therapies New drugs like OPT-302 (Sozinibercept) work alongside traditional anti-VEGF treatments to potentially improve outcomes and extend treatment intervals.
Innovative Approaches for Dry AMD
Photobiomodulation (PBM) Phase 3 trials of this light therapy showed sustained vision improvement and reduced geographic atrophy progression over two years.
Complement Pathway Targeting Beyond the currently approved treatments, multiple new complement inhibitors are in development, offering hope for even more effective dry AMD management.
Oral Medications Several companies are developing oral treatments that could eliminate the need for eye injections:
- ALK-001: An oral vitamin A replacement showing promise for genetic forms of macular degeneration
- LBS-008 (Tinlarebant): Reduces toxic vitamin A byproducts associated with retinal damage
Creating Your Personal AMD Prevention Plan
Given the wealth of information about macular degeneration, creating a personalized approach to vision protection becomes crucial.
Risk Assessment and AMD Screening Schedule
If you’re under 50 with no risk factors:
- Comprehensive eye exam every 2 years
- Begin Amsler grid monitoring if family history exists
If you’re 50-65 with risk factors:
- Annual comprehensive eye exams with OCT imaging
- Consider a nutritional supplementation consultation
- Implement lifestyle modifications
If you’re over 65:
- Annual eye exams with advanced imaging
- Regular Amsler grid monitoring
- Stay current with new treatment developments
Working with Your Eye Care Team
Building a strong relationship with qualified eye care professionals is essential. Look for providers who:
- Offer advanced diagnostic imaging (OCT, fundus photography)
- Stay current with the latest treatment developments
- Provide clear explanations of your condition and options
- Support your questions and concerns
- Coordinate with other healthcare providers when needed
Home Monitoring Strategies
Amsler Grid Testing: Perform monthly at a minimum, weekly if you have intermediate AMD or higher risk. Note any changes in line straightness, missing areas, or distortions.
Symptom Awareness Stay alert for:
- Sudden vision changes
- New dark spots
- Increased difficulty with familiar tasks
- Changes in color perception
Technology Assistance: Consider FDA-approved home monitoring devices like the ForeseeHome Monitor for dry AMD patients who qualify for Medicare coverage.
Lifestyle Modifications: Evidence-Based Prevention Strategies
Research consistently demonstrates that certain lifestyle factors can significantly impact AMD development and progression.
Nutritional Approaches
AREDS2 Diet Principles: Base your eating plan on foods rich in:
- Lutein and Zeaxanthin: Found in dark leafy greens, egg yolks, and corn
- Omega-3 fatty acids: Present in fatty fish, walnuts, and flaxseeds
- Vitamin C: Abundant in citrus fruits, berries, and bell peppers
- Vitamin E: Available in nuts, seeds, and vegetable oils
- Zinc: Found in oysters, beef, and pumpkin seeds
Mediterranean Diet Benefits Studies show that following a Mediterranean-style eating pattern can reduce AMD risk by up to 30%. Focus on:
- Fresh vegetables and fruits
- Whole grains and legumes
- Fish and seafood
- Olive oil as the primary fat source
- Limited red meat and processed foods
Exercise and Cardiovascular Health
Regular physical activity benefits eye health through:
- Improved blood circulation to the retina
- Reduced inflammation throughout the body
- Better management of cardiovascular risk factors
- Weight management
Aim for at least 150 minutes of moderate-intensity exercise weekly, as recommended by major health organizations.
Environmental Protection
UV Protection: Consistent use of UV-blocking sunglasses and wide-brimmed hats may reduce long-term AMD risk. Look for sunglasses that block 99-100% of both UVA and UVB rays.
Blue Light Consideration. While research on blue light’s role in AMD remains inconclusive, some patients benefit from blue light filtering glasses, especially if they experience digital eye strain.
Recent Research Breakthroughs and Clinical Insights
Three significant studies published in 2024-2025 have enhanced our understanding of macular degeneration treatment and prevention.
AREDS2 Follow-up Analysis
A new analysis of data from the National Eye Institute’s (NEI) Age-Related Eye Disease Studies (AREDS and AREDS2) has shown that the AREDS nutritional supplements slowed the progression of geographic atrophy (GA), the late-stage of dry age-related macular degeneration (AMD). Specifically, for the majority in AREDS and AREDS2 who developed GA far from the fovea, the supplements slowed the rate of GA expansion towards the fovea by approximately 55 percent over an average of three years.
Gene Therapy Advancement
REGENXBIO, a clinical-stage gene therapy biotechnology company, is conducting two pivotal, Phase 3 clinical trials for RGX-314, its gene therapy designed to halt the growth of leaky blood vessels that cause retinal degeneration and central vision loss in people with the wet form of age-related macular degeneration (AMD). This represents a potential paradigm shift toward one-time treatments.
Stem Cell Therapy Progress
Luxa Biotechnology reported encouraging results for six patients with dry AMD receiving a low dose (50,000 cells) of RPESC-RPE-4W, its proprietary retinal pigment epithelial stem cell therapy, in a Phase 1/2a clinical trial. Most remarkably, the three patients with worse vision in the clinical trial responded best to Luxa’s emerging RPE stem cell treatment. Their average best corrected visual acuity (BCVA) was approximately 32 letters (slightly better than 20/250) upon enrollment. At 12 months after receiving RPESC-RPE-4W, their vision improved an average of 21.67 letters to about 20/80.
Cost Considerations and Insurance Coverage
Understanding the financial aspects of macular degeneration care helps you plan effectively for treatment.
Insurance Coverage Patterns
Medicare Coverage: Most diagnostic tests and established treatments are covered under Medicare Part B, including:
- Routine eye exams for AMD monitoring
- OCT scans and other diagnostic imaging
- Anti-VEGF injections for wet AMD
- FDA-approved treatments for geographic atrophy
Private Insurance Variables Coverage varies by plan, but most comprehensive policies cover:
- Annual eye exams with AMD risk factors
- Medically necessary treatments
- Some nutritional supplements with proper documentation
Treatment Costs
Anti-VEGF Injections
- Lucentis: $1,800-2,000 per injection
- Eylea: $1,850-2,000 per injection
- Eylea HD: $2,600 per injection
- Avastin: $50-100 per injection (off-label use)
- Vabysmo: $2,000+ per injection
Nutritional Supplements AREDS2 formulations typically cost $20-40 monthly, making them a cost-effective prevention strategy.
Emerging Treatments Gene therapy and stem cell treatments will likely be expensive initially, but may prove cost-effective long-term by reducing the need for ongoing injections.
When to Seek Immediate Medical Attention
Certain symptoms require urgent evaluation to prevent irreversible vision loss.
Emergency Warning Signs
Contact your eye doctor immediately if you experience:
- Sudden appearance of straight lines looking wavy or bent
- Rapid onset of dark or blank spots in central vision
- Sudden decrease in visual sharpness
- Abrupt changes in color perception
- New distortion in familiar objects
The Critical 48-Hour Window
Research indicates that the earlier you start receiving anti-VEGF treatment, the better your outcome is likely to be (one recent study suggests within the first 48 hours of onset). This emphasizes why an AMDF-supported study is showing that time-to-treatment may be the most important factor in preserving your vision.
Future Outlook: What’s Coming Next
The next decade promises unprecedented advances in macular degeneration treatment and prevention.
Emerging Research Areas
Artificial Intelligence Integration: AI-powered diagnostic tools are becoming increasingly sophisticated at detecting early AMD changes, potentially enabling even earlier intervention.
Personalized Medicine Approaches Genetic testing may soon guide individualized treatment selection, optimizing outcomes based on your specific genetic profile.
Nanotechnology Applications Researchers are developing nanosystems for targeted drug delivery, potentially improving treatment effectiveness while reducing side effects.
Combination Therapy Strategies Future treatments will likely combine multiple approaches – perhaps gene therapy with nutritional optimization and targeted medications – for synergistic effects.
Prevention Research
Scientists are investigating whether certain medications already approved for other conditions might prevent AMD development, including:
- Statin medications for cardiovascular health
- Anti-inflammatory drugs
- Diabetes medications with retinal protective effects
Taking Action: Your Next Steps
Armed with comprehensive knowledge about macular degeneration, you can now take proactive steps to protect your vision.
Immediate Actions
- Schedule a comprehensive eye exam if you haven’t had one recently
- Begin home monitoring with an Amsler grid if you’re at risk
- Assess your lifestyle factors and implement changes where possible
- Discuss supplementation with your healthcare provider if appropriate
- Create a vision health file to track your eye health over time
Long-term Strategies
- Establish a relationship with a qualified eye care provider
- Stay informed about new treatment developments
- Maintain healthy lifestyle practices consistently
- Consider participating in research if eligible
- Build a support network of family and friends aware of your eye health
Clinical Practice Recommendations and Patient Management
Evidence-Based Screening Protocols
Risk-Stratified Examination Schedules:
Low-Risk Patients (<50 years, no family history):
- Comprehensive ophthalmologic examination every 2-3 years
- Baseline macular photography for future comparison
Intermediate-Risk Patients (50-65 years with risk factors):
- Annual comprehensive examination with OCT imaging
- Amsler grid monitoring initiation
- Nutritional counseling regarding AREDS2 supplementation
High-Risk Patients (>65 years or genetic predisposition):
- Biannual ophthalmologic evaluation with multimodal imaging
- Home monitoring device consideration (ForeseeHome for eligible patients)
- Collaborative care with retinal specialists
Treatment Decision-Making Framework
- Early Stage: Lifestyle modification emphasis, AREDS2 supplementation consideration
- Intermediate Stage: Mandatory AREDS2 supplementation, enhanced monitoring frequency
- Geographic Atrophy: Complement inhibitor therapy evaluation, low vision rehabilitation services
Wet AMD Management:
- Acute Presentation: Emergent anti-VEGF therapy within 24-48 hours
- Chronic Management: Individualized injection schedules based on disease activity
- Treatment-Resistant Cases: Alternative anti-VEGF agents, combination therapy consideration
Additional Resources and Citations
Based on the research conducted for this article, here are three key authoritative sources that provide additional depth and current information on macular degeneration:
1. CDC Vision and Eye Health Surveillance System (VEHSS)
Link: https://www.cdc.gov/vision-health-data/prevalence-estimates/amd-prevalence.html
This comprehensive database provides the most current prevalence estimates of AMD in the United States, including state and county-level data. The VEHSS contains modeled estimates showing that 19.8 million Americans aged 40+ live with some form of AMD, with detailed demographic breakdowns and geographic variations. This resource is particularly valuable for understanding the scope of AMD impact and planning preventive care strategies.
2. American Macular Degeneration Foundation – 2025 AMD Awareness Resources
Link: https://www.macular.org/amdawarenessmonth
The AMDF provides current statistics, patient education materials, and updates on the latest research developments. Their 2025 awareness resources include information about the critical 48-hour treatment window for wet AMD, risk reduction strategies, and home monitoring tools like the Amsler grid. The foundation also maintains a research participant database for those interested in clinical trials.
3. Foundation Fighting Blindness – AMD Research Advances
Link: https://www.fightingblindness.org/news/age-related-macular-degeneration-research-advances-821
This resource provides detailed information about cutting-edge treatments currently in development, including gene therapy trials (RGX-314), stem cell research (Luxa Biotechnology’s RPESC-RPE-4W), and FDA-approved treatments for geographic atrophy (SYFOVRE and Izervay). The foundation tracks clinical trial progress and breakthrough therapies that may transform AMD treatment in the coming years.
These resources were selected based on their scientific authority, currency of information, and relevance to both patients and healthcare providers seeking comprehensive AMD information.
Conclusions and Future Directions
Macular degeneration management has undergone substantial advancement, transitioning from purely observational care to active therapeutic intervention. Current evidence supports early detection initiatives, risk factor modification, and prompt treatment implementation as key strategies for vision preservation.
The therapeutic landscape continues evolving rapidly, with gene therapy, stem cell interventions, and extended-duration treatments offering promise for improved patient outcomes. Healthcare providers should remain informed regarding emerging therapies while maintaining focus on proven interventions, including nutritional supplementation, lifestyle modification, and timely anti-VEGF therapy.
Early detection remains the cornerstone of effective AMD management. Regular ophthalmologic evaluation, particularly for individuals with established risk factors, enables optimal therapeutic timing and maximizes visual preservation potential. The integration of advanced imaging technologies with traditional clinical assessment provides unprecedented capability for disease monitoring and treatment optimization.
Contemporary research developments suggest that the traditional paradigm of AMD as an inevitable consequence of aging may be challenged by emerging therapeutic modalities. Gene therapy and regenerative medicine approaches offer potential for disease modification rather than symptom management alone.
Healthcare systems should prioritize AMD screening protocols, ensure timely specialist access, and maintain current knowledge regarding rapidly evolving treatment options to optimize patient outcomes in this prevalent condition affecting millions of Americans.
FAQs
-
Early signs include blurry central vision, difficulty recognizing faces, dark spots in vision, wavy straight lines, and colors appearing less vibrant.